- 4192 Devonwood Way, Ashburn, Virginia, 20148
- Helpline: +1 (703) 665-3747
Neonatal Major Thromboembolic Event: Challenging in Diagnosis and Treatment
- Home
- Back to Journal
- Article Details
Abstract
Neonatal purpura fulminans is a rare and rapidly progressive life-threatening disease that occurs secondary to acute disseminated intravascular coagulation and hemorrhagic necrosis of the skin. Here we described a newborn that developed purpura fulminans of the left leg at 16 hours of age with a normal thrombophilia screen. The infant was transferred to the neonatal intensive care unit at King Saud University Medical City (King Khaled University Hospital) and treated with Heparin bolus followed by infusion along with other supportive measures. With aggressive management, the left leg improved dramatically, and the baby was discharged home in good health on low molecular weight heparin. The left foot underwent autoamputation one-month post-discharge from the intensive care unit.
Keywords: Newborn; Purpura; fulminans; Congenital; Protein deficiency; thrombosis; coagulopathy; anticoagulant
Introduction
Thromboembolic events are being more recognized and diagnosed in the pediatric age group [1]. Among children, neonates are more susceptible to develop symptomatic venous thrombosis, with an incidence of 5.1 cases per 100,000 live births [2].
Newborns have a distinct hemostatic system in terms of quantity and quality compared to older children and adults [3]. The tendency to develop thrombosis in the neonatal period may arise from inherited or acquired factors and may vary in presentation from being asymptomatic to being life-or limb-threatening [4]. Moreover, with the lack of evidence- based guidelines, it is challenging for the neonatologist to manage such cases.
Here we are reporting a case of Saudi neonate who developed neonatal purpura fulminans in the left lower limb shortly after birth with a normal thrombophilia screen, which constitutes a challenge in diagnosis and management.
Case Report
A Saudi male was born at term by an elective cesarean section with an APGAR score of 6 and 8 at 1st & 5th minutes, respectively, following a smooth antenatal course. This baby was the second child for healthy parents with third-degree consanguinity. There was no history thrombophilic event or any hematological disease in the family. The baby developed secondary apnea, so he was given positive pressure ventilation then admitted to the Neonatal Intensive Care Unit (NICU) on non-invasive mechanical ventilation. His respiratory distress was worsening, so he was intubated and given two doses of surfactant. Partial sepsis screen done then started on broad-spectrum antibiotics. No umbilical arterial catheterization was reported and no inotropic support. At 16 hours of age, the baby developed a pale and pulseless left leg. Urgent doppler US done showed echogenic thrombus with lumen occlusion at the distal aspect of the external iliac artery & femoral artery. He was given Immediately Heparin Bolus 260 IU over 10 minutes, followed by continuous Infusion 28 unit/kg/hr. No focal neurological deficits or seizures and no hematuria. Both cranial & abdominal ultrasound was reported normal.
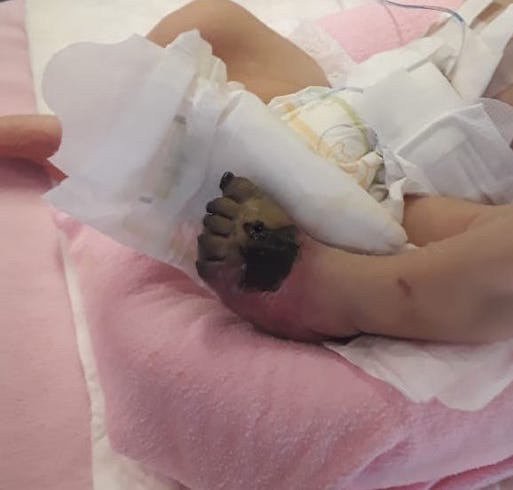
Over the next two days, the color changed to bluish involving distal 1/3 left foot with mild ecchymosis of the left buttock (Figure 1). The vascular surgeon was consulted and advised for urgent referral to a higher surgery center for catheterization and thrombectomy, and further thrombophilia and genetic workup.
Figure 1: Shows a well-defined gangrenous plaque over the dorsum of the left foot and gangrenous toes
The patient was transferred to our center at King Saud University Medical City (KSUMC) & King Khaled University Hospital (KKUH). Laboratory values from the referring hospital reported normal platelet count, Protein C 27% (normal range 20–64%), and Antithrombin III 22% (normal range 39–87%).
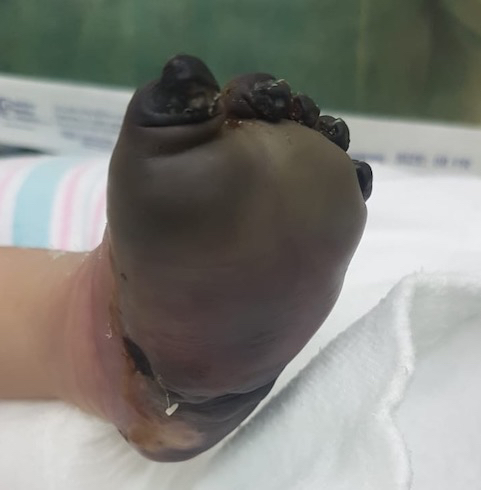
The baby was admitted in our NICU connected to mechanical ventilation, with stable gas and vital signs, and a physical examination showed a gangrenous left foot (Figure 2). He was managed by a multidisciplinary team as left lower limb major thromboembolic phenomena in the femoral and popliteal artery. Repeated thrombophilia screen showed normal platelets with normal coagulation profile. Protein C level was 53%; Protein S Total 51% and Antithrombin III 66%, all of which were normal for his age. Factor V Leiden & Factor II Mutation by molecular genetics was negative. Other laboratory tests, including serum electrolytes, renal functions, liver functions, blood cultures, and virology screening all were normal. The baby also underwent echocardiography and CT brain to rule out any abnormality, and both were normal. Doppler ultrasound showed no blood flow in the left popliteal artery, posterior tibial artery, and dorsalis pedis. The baby was initially started on heparin infusion then shifted to Low Molecular Weight Heparin (LMWH) subcutaneous injections 1 mg/kg BID by a pediatric hematologist. Vascular Surgery, at this point, recommended no surgical/vascular intervention and continues conservative management till the foot undergoes auto-amputation. The patient was on broad-spectrum antibiotics, and a nitroglycerin patch was applied over the distribution of the posterior tibial artery of the left foot to improve the perfusion.
Figure 2: Shows total necrotic left foot upon admission to our NICU
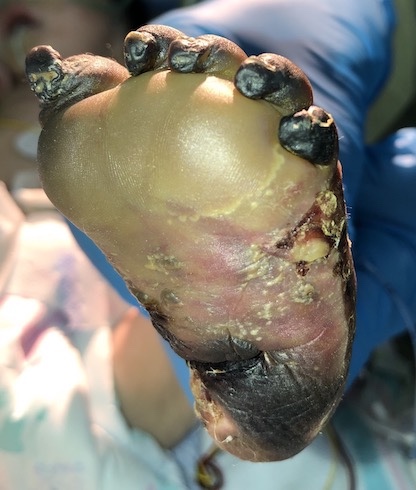
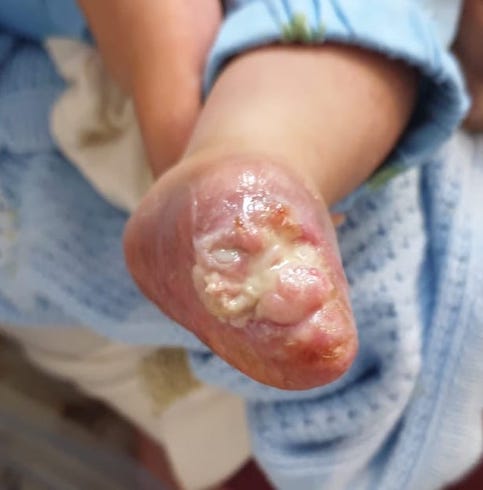
After five days of therapy, the left foot showed dramatic improvement and healed without any signs of infection and no new infarcts (Figure 3). The baby was discharged after 30 days of hospitalization on a prophylactic dose of LMWH 4.5 mg once daily for three months. After four weeks of discharge, the left foot underwent self-amputation (Figure 4).
Figure 3: shows improvement after five days of therapy
Figure 4: Shows left foot after undergoing auto-amputation four weeks post-discharge
Discussion
Thromboembolism is relatively rare in the pediatric population, but neonates are at the highest risk of developing such events [5]. The incidence of neonatal thrombophilia is trending up, especially in the critically ill neonate, due to the prematurity of their hemostatic mechanisms and interaction with external factors such as sepsis and invasive medical procedures [6].
The causes could be inherited or acquired. Inherited causes are commonly due to homozygous protein C/S deficiency (quantitative) or functional protein defect (qualitative). Others such as Factor V Leiden or antithrombin deficiency [7,8]. Acquired causes are more frequent and often associated with sepsis and secondary consumptive coagulopathy or procedures such as complicated central catheterization [9].
Here we report the case of a Saudi male newborn that developed a left lower limb thromboembolic event soon after birth while having a thrombophilia screen within normal ranges for his age. It raises the matter of having a functional anticoagulant protein defect rather than an actual deficiency, or a possible unreported central catheterization.
Worldwide, there are several cases of purpura fulminans reported during 1985 and 2019. All patients reported presented with necrotic lesions in the scalp and extremities during the first few days of life [10–17]. Homozygous protein C mutation was detected in patients with a history of consanguineous parents [10], whereas heterozygous mutation was found in newborns of unrelated parents [11,14,17,18]. Findley T et al. reported a newborn who had similar presentation and outcome as in our case but found to have undetectable levels of protein C with negative genetic testing [16].
The prevalence of neonatal thrombophilia is still unknown in the Middle East and Arab countries. In Saudi Arabia, there are 6 case reports of neonatal purpura fulminans from 2002 to 2017. Two of the reported cases were secondary to hereditary homozygous protein C gene mutation, while the rest of the cases didn’t undergo genetic evaluation [19,20]. Purpura Fulminans most commonly presented as intracranial hemorrhage and blindness secondary to retinal detachment and vitreous hemorrhage [19–22]. Another case was secondary to group B streptococcus sepsis [23]. In all cases, there were positive consanguineous marriages. All cases reported unfavorable outcomes (blindness, seizure, hydrocephalus, cerebral palsy, and death). On the contrary, our patient has a good outcome, and he survived until discharge.
In conclusion, it is essential to acknowledge that healthy term neonates show reduced and highly variable physiological levels of natural anticoagulants such as protein C and protein S [24]. Some neonates may become symptomatic and develop purpura fulminans while others don’t, which could be attributed to a functional defect in a natural anticoagulant protein rather than a decrease in its number. Reporting such cases from the Arab region where consanguineous marriage rate is high is crucial in detecting and treating such a disease.
References
- Nowak-Gottl U, During C, Kempf-Bielack B, et al. (2003)Thromboembolic diseases in neonates and children. Pathophysiology Haemost Thromb 33: 269–274. [View]
- Corrigan J (1992) Normal hemostasis in fetus and newborn: coagulation. In: Fetal and neonatal physiology. Saunders WB; Pg No: 1368–1371.
- Andrew M (1995) Developmental Hemostasis: Relevance to thromboembolic complications in pediatric patients. Thromb Haemost 74: 415–425. [View]
- Saracco P, Bagna R, Gentilomo C, Magarotto M, Viano A, et al. (2016) Clinical data of neonatal systemic thrombosis. J Pediatr 171: 1. [View]
- Raffini L, Huang YS, Witmer C, Feudtner C (2009) Dramatic increase in venous thromboembolism in children’s hospitals in the United States from 2001 to 2007. Pediatrics 124:1001–1008. [View]
- Andrew M, David M, Adams M, Ali K, Anderson R, et al. (1994) Venous thromboembolic complications (VTE) in children: first analyses of the Canadian Registry of VTE. Blood 83: 1251–1257. [View]
- Reitsma PH, Bernardi F, Doig RG, Gandrille S, Greengard JS, et al. (1995) Protein C deficiency: a database of mutations, 1995 update. Thromb Haemost 73: 876–889. [View]
- Dogan Y, Aygun D, Yilmaz Y, Kanra G, Secmeer G, et al. (2003) Severe protein S deficiency associated with heterozygous factor V Leiden mutation in a child with purpura fulminans. Pediatr Hematol Oncol 20: 1–5. [View]
- Hermansen MC, Hermansen MG (2005) Intravascular catheter complications in the neonatal intensive care unit. Clin Perinatal 32: 141–156. [View]
- Marciniak E, Wilson HD, Marlar RA (1985) Neonatal purpura fulminans: a genetic disorder related to the absence of protein C in blood. Blood 65(1):15–20. [View]
- Sen K, Roy A (2006) Management of neonatal purpura fulminans with severe protein C deficiency. Indian Pediatrics 43: 542–545. [View]
- Saeidi R, Gharaee R, Nobakht Z (2014) Neonatal Purpura Fulminans. Iranian Journal of Neonatology IJN 5: 34–37. [View]
- Sharma S, Anbazhagan J, Plakkal N (2015) Neonatal purpura fulminans due to protein C deficiency Arch Dis Child Fetal Neonatal Ed 100: F453. [View]
- Shah R, Ferreira P, Karmali S, Le D (2016) Severe Congenital Protein C Deficiency: Practical Aspects of Management. Pediatr Blood Cancer 63: 1488–1490. [View]
- Kizilocak H, Ozdemir N, Dikme G, Koc B, Celkan T (2018) Homozygous protein C deficiency presenting as neonatal purpura fulminans: management with fresh frozen plasma, low molecular weight heparin and protein C concentrate. J Thromb Thrombolysis 45: 315–318. [View]
- Findley T, Patel M, Chapman J, Brown D, Duncan AF (2018) Acquired Versus Congenital Neonatal Purpura Fulminans: A Case Report and Literature Review. J Pediatr Hematol Oncol 40: 625–627. [View]
- Zhang H, Bi X, Su Z, Tu X, Wang L, Shen B (2018) A novel compound heterozygous mutations in protein C gene causing neonatal purpura fulminans. Blood Coagul Fibrinolysis 29: 216–219. [View]
- Watanabe K, Arakawa Y, Yanagi M, Isobe K, Mori M, et al. (2019) Management of severe congenital protein C deficiency with a direct oral anticoagulant, edoxaban: A case report. Pediatr Blood Cancer 66: 27686. [View]
- Abu-Amero KK, Al-Hamed MH, Al-Batniji FS (2003) Homozygous protein C deficiency with purpura fulminans: report of a new case and a description of a novel mutation. Blood Coagulation & Fibrinolysis 14: 303–306. [View]
- Al-Hamed MH, Albatniji F, Aldakheel GA, El-Faraidi H, Al-Zahrani A, et al. (2016) Molecular characterization of novel splice site mutation causing protein C deficiency. Blood Coagulation & Fibrinolysis 27: 585–588. [View]
- M Abdellatif, M Al Bakrah, M Qureshi, A Al-Nemri (2007) Protein C deficiency in a neonate with purpura fulminans. The Internet Journal of Pediatrics and Neonatology 8: 2. [View]
- Al Hawsawi ZM, Alhejaili AA, Mohy Uddin M, Abdelkarim ME (2016) Hereditary protein C deficiency in a Saudi neonate with bilateral adrenal gland hemorrhages: A rare case report. J Taibah Univ Med Sc 11:485–488. [View]
- AlBarrak M, Abdulrahman Al-Matary (2013) Neonatal purpura fulminans manifestation in early-onset group B Streptococcal infection. Am J Case Rep 14: 315–317. [View]
- Williams MD, Chalmers EA, Gibson BE (2002) Hemostasis and Thrombosis Task Force, British Committee for Standards in Hematology. The investigation and management of neonatal hemostasis and thrombosis. Br J Haematol 119: 295–309. [View]
Article Type
Case Report
Publication history
Received: September 02, 2024
Accepted: September 15, 2024
Published: September 17, 2024
Citation:
Najd S. Musibeeh NS, AlNemri AM (2024) Neonatal Major Thromboembolic Event: Challenging in Diagnosis and Treatment. Cancer Stud and Therap I 05(01): 134–138.
Najd S. Musibeeh*1 and Abdulrahman M. AlNemri2
1Pediatric Resident, Department of Pediatrics, College of Medicine King Saud University Kingdom of Saudi Arabia
2Professor of Pediatrics & Consultant Neonatologist, Department of Pediatrics, College of Medicine King Saud University Kingdom of Saudi Arabia
*Corresponding author
Najd S. Musibeeh,
Pediatric Resident,
Department of Pediatrics,
College of Medicine,
PO Box. 2925, Riyadh 11461,
Kingdom of Saudi Arabia;
Phone: 00966-11-4671099;
Fax: 00966-11-4671709;
E-mail: nmusibeeh@ksu.edu.sa
Najd S. Musibeeh*1 and Abdulrahman M. AlNemri2
1Pediatric Resident, Department of Pediatrics, College of Medicine King Saud University Kingdom of Saudi Arabia
2Professor of Pediatrics & Consultant Neonatologist, Department of Pediatrics, College of Medicine King Saud University Kingdom of Saudi Arabia
*Corresponding author
Najd S. Musibeeh,
Pediatric Resident,
Department of Pediatrics,
College of Medicine,
PO Box. 2925, Riyadh 11461,
Kingdom of Saudi Arabia;
Phone: 00966-11-4671099;
Fax: 00966-11-4671709;
E-mail: nmusibeeh@ksu.edu.sa